Positive results from Targovax’s skin cancer study
Our member Targovax announced an update from the company’s clinical study on melanoma patients this week.
The clinical study offers Targovax’s medicine ONCOS-102 in combination with the checkpoint inhibitor Keytruda to skin cancer patients with serious disease progression. The patients were all at Stage III and Stage IV at the beginning of the trial and had been through the standard of care. They had no other treatment options after failing anti-PD-1 treatment.
What is anti-PD1 treatment?
PD-1 is a protein that is found on T cells (a type of white blood cell that is part of the immune system) that helps keep the body’s immune responses under control. When PD-1 binds to another protein called PD-L1, which can be found on normal cells and in higher amounts on some cancer cells, it keeps the T cells from destroying cells, including cancer. Some anti-cancer drugs called immune checkpoint inhibitors are used to block PD-1. This releases the brakes on the immune system and increases the ability of T cells to kill cancer cells.
Checkpoint inhibitors have revolutionized the treatment of cancer in the last ten years, but they do not work on all cancer patients. Some patients do not have the right types of T cells for the treatment to work. The oncolytic virus called ONCOS-102 developed by Targovax is a combination product, which tricks the immune system to produce these T cells that can help destroy cancer cells.
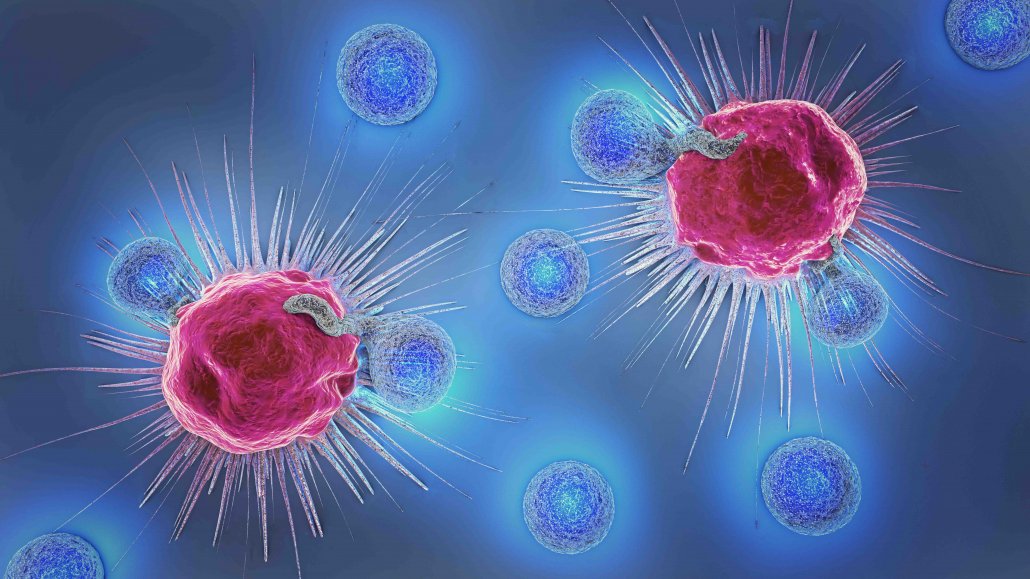
Illustration of cancer cells under attack from lymphocytes (white blood cells), part of the immune system.
Partial or complete responses
According to the newly released data from Targovax, 7 of the 20 patients in the clinical study had partial or complete responses after receiving the combination treatment of the immune checkpoint inhibitor Keytruda and the oncolytic virus ONCOS-102. The patients had overall more than a 30 per cent reduction of their tumours. One patient had a complete response, while the overall response rate was 35 per cent.
Systemic effects
Two patients had a response in non-injected lesions. This means that a response was observed in melanoma lesions that had not been injected with the oncolytic virus. This is what is known as a systemic effect and has not been seen with oncolytic viruses before. Two non-injected lesions had completely disappeared on the patients in the study group.
“These impressive efficacy data in anti-PD1 refractory melanoma are the most important clinical results for Targovax to date,” Øystein Soug, Chief Executive Officer of Targovax, commented.
“The data clearly confirm our hypothesis that ONCOS-102 can benefit cancer patients resistant to checkpoint inhibition by triggering local and systemic immune activation,” Soug continued. “They also provide evidence of clinical efficacy and establishes ONCOS-102 as one of the most promising combination partners to checkpoint inhibitors. We will now carefully analyze the immunological data and are planning for a confirmatory melanoma trial for the ONCOS-102 and checkpoint inhibitor combination.”
- For more information, please read the press release from Targovax or visit the company’s website.













